
Mental Health & The Menstrual Cycle: Connecting FAM + Mental Wellness
Often overlooked but vital, the menstrual cycle speaks volumes about your health. In recent years,

Your body is constantly communicating with you… You just need to learn its language. Body literacy is about understanding the biological signs and signals your body sends throughout your menstrual cycle, giving you agency over your reproductive health and life choices.
One of the most powerful tools in body literacy? Learning to observe and interpret your cervical fluid.
Cervical fluid changes throughout your cycle in predictable, meaningful ways. Whether you’re trying to conceive, preventing pregnancy without hormones, monitoring your hormone health, or simply wanting to understand how your body works, cervical fluid observation puts knowledge and power in your hands.
In this guide, we’ll explore how cervical fluid changes throughout your cycle, what different types look and feel like, and how to interpret what you’re observing.
This is body literacy in action: learning to read your body’s fertility signals so you can make informed decisions about your fertility and health.
Your cervix produces fluid throughout your menstrual cycle and this cervical fluid changes dramatically in consistency and appearance as your hormones shift.
Side Note: You may see some sources call this “cervical mucus,” but I often use the term cervical fluid. It’s analogous to seminal fluid, a substance with a similar reproductive function and helps normalize this natural bodily function.
Why does this matter?
Because these changes can tell you exactly where you are in your cycle and can support you whether you’re avoiding getting pregnant or trying to conceive (TTC).
Fertility awareness educators often reference classifications developed by Dr. Erik Odeblad, who identified different types of cervical fluid based on how they’re produced in the cervix and how they function throughout the menstrual cycle. While these types are identified scientifically, what you notice day-to-day is based on observable patterns influenced by hormones.
Here’s an overview of the main types and how they relate to fertility:
Note: The following pictures are for reference only.
G-type (Gestagenic / Barrier mucus)
L-type (Lubricative / Filtering mucus)
S-type (Stretchy / Transportive mucus)
P-type (Peak-phase mucus)
| Mucus Type | Typical Hormonal Influence | Fertility Relevance | Notes |
|---|---|---|---|
| G mucus | Progesterone | ❌ Low | Thick barrier, not conducive to sperm. |
| L mucus | Estrogen rising | ⚠️ Moderate | Intermediate; can filter sperm. |
| S mucus | High estrogen | ✔️ Fertile | Supports sperm transport. |
| P mucus | Estrogen peak/transition | ✔️ Fertile around ovulation | Smaller amounts, multiple subtypes. |
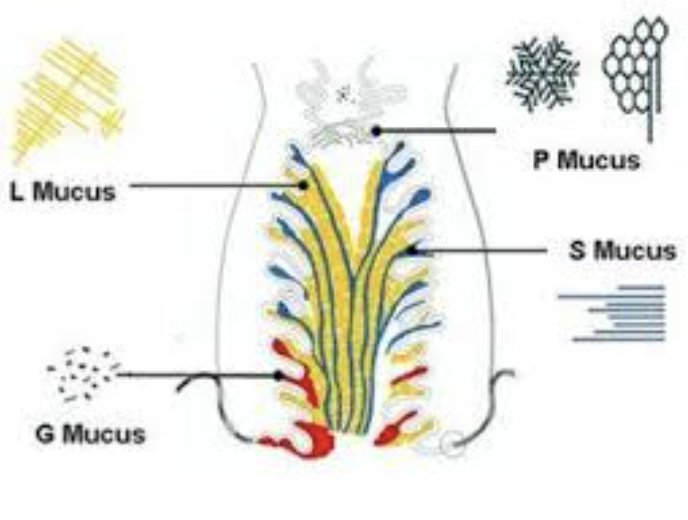
A Very Important Note: In real life, you may observe combinations of these qualities rather than one distinct “type” at a time. Fertility awareness methods often focus on what you can feel and see (wetness, slipperiness, stretchiness) rather than trying to match observations perfectly to microscopic fluid/mucus categories.
You might also hear cervical fluid described in these everyday terms:
Check toilet paper after wiping, or insert a clean finger into your vagina to collect a sample. Pay attention to how it looks, feels, and stretches between your fingers. Record your observations in a fertility tracking app or chart to identify patterns over time.
As you become familiar with these changes, you’ll start recognizing your own patterns and understanding when you’re most fertile.
Cervical fluid isn’t just a side effect of your cycle. It’s an active participant in conception. The presence and quality of your cervical fluid significantly impacts your chances of getting pregnant.
As your body prepares for ovulation, rising estrogen levels trigger your cervix to produce increasingly fertile fluid. This fluid:
Outside your fertile window, cervical fluid becomes thick and sticky (or may be absent entirely). This creates a barrier that prevents sperm from reaching the egg, which is why fertility awareness can work as natural birth control when used correctly.
The right type of cervical fluid provides nutrients, protection, and a clear pathway for sperm. Hostile or absent cervical fluid can impede sperm motility and reduce fertilization chances. By learning to observe and interpret these changes, you gain valuable insights into your fertility window.
Your cervical fluid doesn’t change randomly. It follows a predictable pattern driven by your hormones.
Here’s what typically happens:
Your period arrives, lasting about 3-7 days. During menstruation, you won’t be able to observe cervical fluid because bleeding obscures it.
After your period ends, you might experience a few “dry” days with little or no cervical fluid. As follicle-stimulating hormone (FSH) prompts your ovaries to prepare an egg, estrogen begins rising.
This is when you’ll notice cervical fluid transitioning from dry or sticky to creamy, then increasingly wet and slippery. This fertile window typically lasts 3-5 days.
As ovulation nears, rising estrogen causes your cervical fluid to become clear, stretchy, and slippery… that classic “egg white” consistency. This is your most fertile cervical fluid and indicates your highest chance of conception.
After ovulation, progesterone takes over. Your cervical fluid (now called luteal mucus) quickly becomes thick and sticky again, or dries up entirely. This marks the end of your fertile window and continues until your next period.
By tracking these patterns for a few cycles, you’ll learn your unique rhythm and can identify your fertile window with increasing accuracy.
If you’re new to observing cervical fluid, you probably have questions. Let’s clear up some common misconceptions:
Not necessarily. Some women produce less noticeable cervical fluid, while others have abundant, obvious changes. If you’re having trouble observing it externally, try checking internally with a clean finger. Also, certain medications (like antihistamines) and dehydration can reduce cervical fluid production.
No. While cervical fluid is most abundant and fertile around ovulation, you may observe different types throughout your entire cycle. Even less-fertile types provide information about where you are in your cycle.
This depends entirely on the method and how consistently you use it. Modern fertility awareness methods, when used correctly with proper education, can be highly effective. The symptothermal method (which combines cervical fluid observation with temperature tracking) has a perfect-use effectiveness rate of about 99%, though typical use effectiveness ranges from 77-98% depending on the specific method and consistency of use.
The key?
Work with a certified fertility awareness educator who can teach you to accurately observe and interpret your signs.
Let’s recap what we’ve covered:
Understanding your cervical fluid empowers you to take an active role in your reproductive health. Whether you’re trying to conceive, avoiding pregnancy naturally, or simply want to understand your body better, cervical fluid observation is a valuable skill.
Start by simply observing for a few cycles without pressure. Notice the patterns. Track what you see. Over time, you’ll develop confidence in reading your body’s signals and can make informed decisions about your fertility.
Ready to start your fertility awareness journey? Consider connecting with a certified fertility awareness educator, like myself, who can guide you through the learning process and answer your specific questions.
Disclaimer:
The information provided on this blog is for educational and informational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. The content on this blog is not meant to replace professional medical advice or to be used to prevent, diagnose, or treat any disease or illness. Reliance on any information provided by this blog is solely at your own risk.

Often overlooked but vital, the menstrual cycle speaks volumes about your health. In recent years,

In today’s world, more women are seeking natural and safe methods to enhance their understanding

Exploring the connection between fertility awareness and birth control can seem overwhelming given the myriad

You’ve probably heard of environmental toxins. Whether it’s concerns raised over what is sprayed on

Do you notice shifts in energy levels, moods, and cravings throughout your menstrual cycle? Many

If you’re looking to enhance your reproductive health or gain a better understanding of fertility
Sign up today and receive your FREE Resource Bundle to support your journey towards hormone health, fertility, gut wellness, cycle wisdom, and holistic nutrition!